NMN supplementation protects mice from inflammatory bowel disease
Researchers from Ajou University School of Medicine in South Korea helped elucidate the mechanisms of inflammation and inflammatory bowel disease by finding that levels of NAD+ correlated with the severity of inflammatory bowel disease in mice. In a study published in the journal Redox Biology, mice lacking the enzyme NAMPT, which produces the NAD+ precursor NMN, in their macrophages increased the severity of inflammatory bowel disease in response to inflammation while reducing survival Rate.
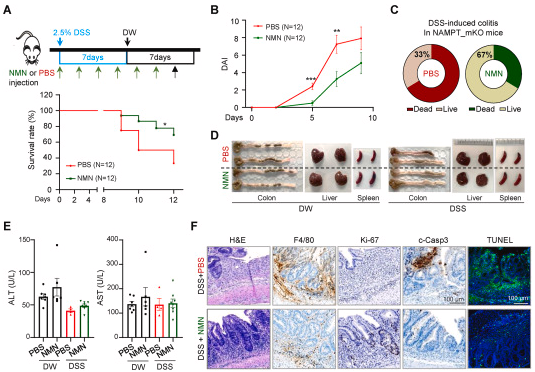
These effects, including disease severity and survival, were restored by injecting mice with NMN (500 mg/kg body weight three times a week). These findings suggest that activation of the NAMPT-dependent NAD+ biosynthetic pathway may potentially treat inflammatory diseases such as inflammatory bowel disease.
Our gut is a metabolic metropolis filled with a multitude of microbes and cells. One of these cells, macrophages, plays a key role in regulating the immune system of the intestinal mucosa. The function of these intestinal macrophages is to remove pathogens, bacterial wall components and dead cells.
However, failure to mount a strong protective response to pathogens during the resolution phase of inflammation may lead to persistent and excessive inflammation, which is a common condition in inflammatory bowel disease. In addition, accumulating evidence suggests that enhanced resolution of inflammation in macrophages may be a new therapeutic approach to control intestinal inflammation and restore tissue function.
To investigate the role of NAMPT in inflammatory bowel disease, the researchers and colleagues induced inflammatory bowel disease in mice that lacked a functional NAMPT gene in their macrophages. This genetic alteration caused the mice to suffer persistent severe inflammation, and the initial inflammatory response was maintained despite the lack of NAMPT activity. Mice deficient in these macrophage NAMPT also exhibited substantial weight loss and lower survival rates.
The researchers next placed excised skin from these mice into petri dishes (explants) to assess the skin's ability to regenerate. They found that not only was regeneration inhibited, but cell proliferation was also reduced. Since cell proliferation is necessary to generate new skin cells, these findings suggest that wound healing in older mice is slower due to reduced cell proliferation.
The researchers next placed excised skin from these mice into petri dishes (explants) to assess the skin's ability to regenerate. They found that not only was regeneration inhibited, but cell proliferation was also reduced. Since cell proliferation is critical for skin regeneration, these findings suggest that a deficiency in NAD+ may be responsible for hindered skin regeneration.
Overall, this study demonstrates that NMN supplementation protects mice from inflammatory bowel disease, possibly through enhanced resolution of inflammation. However, the clinical translational relevance of this study appears to be limited, as it is unlikely that conditions associated with "macrophage-specific NAMPT depletion" will be encountered in a clinical setting. However, this study highlights the importance of NAD+ in the cleanup activities of macrophages and the subsequent resolution of inflammation.
*Special note - This article is for informational purposes only and cannot replace a doctor's treatment diagnosis and advice. It should not be regarded as a recommendation or proof of efficacy of the medical products involved. If it involves disease diagnosis, treatment, and rehabilitation, please be sure to go to a professional medical institution to seek professional advice.
by GSHWORLD
GSH Bio Tech is China Biological API Manufacturer. China NMN powder suppliers & best NMN raw material Factory.













