Enhancing NAD+ Can Restore Age-Related Muscle Degeneration in Human Cells
Aging is characterized by the imbalance of proteins — disrupted proteostasis — and mitochondrial function. These features are often seen in age-related degenerative disorders characterized by detrimental protein aggregation like Alzheimer’s disease and inclusion body myositis (IBM), a progressive muscle disorder. However, how proteostasis collapses in aging muscle is not fully known, and it is unclear whether harmful protein clumps called amyloid deposition, a hallmark of Alzheimer’s disease and IBM, is also at play in the aging muscle.
Romani and colleagues from the Ecole Polytechnique Fédérale de Lausanne in Switzerland published an article in Cell Reports showing that, during natural aging across species, muscle tissues accumulate amyloid-like deposits. Moreover, the researchers discovered the reversible nature of these deposits, which can be reduced by interventions aimed at restoring mitochondrial homeostasis, such as by enhancing nicotinamide adenine dinucleotide (NAD+) metabolism, even at the onset of aging.
Importantly, they show that reduction of the accumulation of amyloid-like deposits in aging with NAD+ boosters is sufficient to improve muscle mitochondrial function and beneficially impact health- and lifespan. “Drugs that boost mitochondrial quality control could therefore be tested in the clinic to reversion these age-related proteotoxic aggregates and rejuvenate tissues,” says Mario Romani, the first author of the study, in a press release.
Amyloid aggregate accumulation in aging muscle cells across species
Romani and colleagues found that gene activity signatures linked with protein balance and aggregation and with mitochondria are altered in muscle during aging or diseases. They looked at data from a collection of human muscle datasets of aging, genetic muscle diseases like muscle dystrophies, and muscle proteinopathies, such as IBM and amyotrophic lateral sclerosis (also known as Lou Gherig’s disease). Interestingly, amyloidosis and protein-misfolding-related gene sets were among the most consistently induced in all the muscle aging and disease conditions analyzed.
Moreover, Romani and colleagues show accumulation of amyloid-like deposits and mitochondrial dysfunction during natural aging in the body wall muscle of roundworms called nematodes, human primary myotubes (mature muscle cells), and mouse skeletal muscle, partially modeling IBM. Also, they have demonstrated a critical role of NAD+ homeostasis to control amyloid aggregates levels
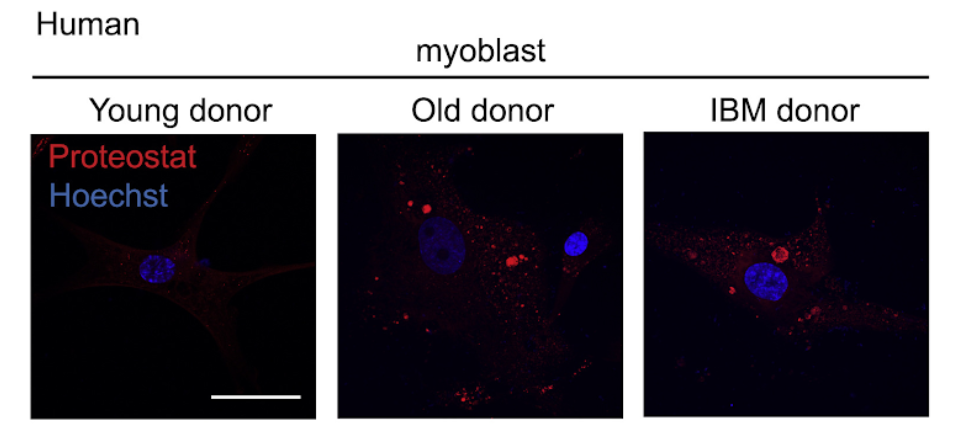
These analyses suggest that there is an overall decline of mitochondrial function paired with perturbed cellular proteostasis in skeletal muscle in established proteinopathies, such as IBM, in aging, as well as in other chronic muscle conditions, including muscular dystrophies. These shared alterations, suggestive of increased protein misfolding and amyloidosis hence may represent a major common hallmark of muscle aging and disease. “These abnormal proteotoxic aggregates could serve as novel biomarkers for the aging process, beyond the brain and muscle,” says Auwerx.
NAD+ boosting reduces amyloid formation and improves mitochondria during aging in worms and mammals
Romani and colleagues also established that the evolutionarily conserved processes of amyloidosis and aging-associated loss of proteostasis are directly linked to levels of NAD+ — a vital molecule with roles in regulating cellular energy, function, and health that declines with age. Since NAD+ balance is critical to control age-associated muscle amyloidosis, Romani and colleagues treated nematodes modeling amyloid-beta muscle proteotoxicity, human aged myotubes, and old mice with the NAD+ boosters nicotinamide riboside (NR) and olaparib (AZD). They then tested for effects on mitochondrial function, muscle homeostasis, and amyloid plaque accumulation.
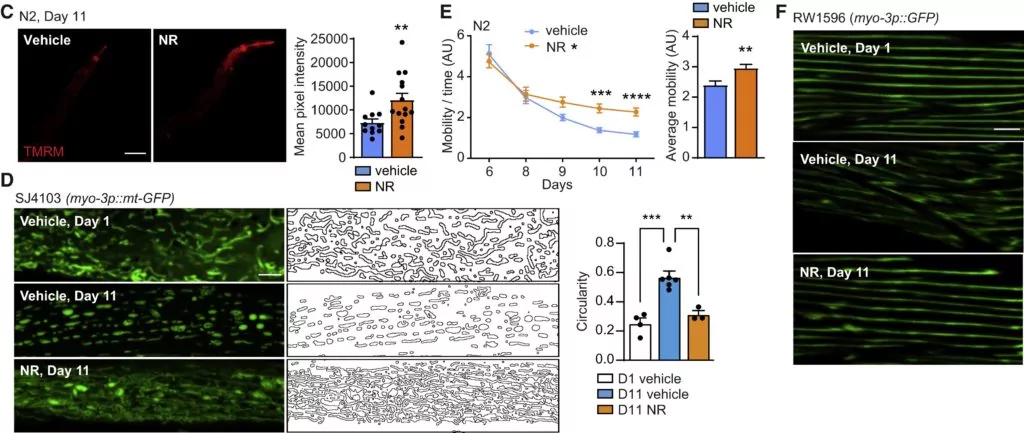
Late-life treatment with either NR (1 mM) or olaparib (AZD; 300 nM) had a profound effect on proteostasis in aged worms, with amyloid-like deposit levels being reduced by both compounds. Late-life NAD+ boosting interventions also restored mitochondrial form and membrane potential — an indicator of membrane functional integrity — in aged animals and increased mitochondrial DNA content, indicative of increased mitochondrial proliferation (biogenesis). This furthermore improved fitness, measured as spontaneous movement, muscle integrity, and percentage of paralysis and death at day 18.
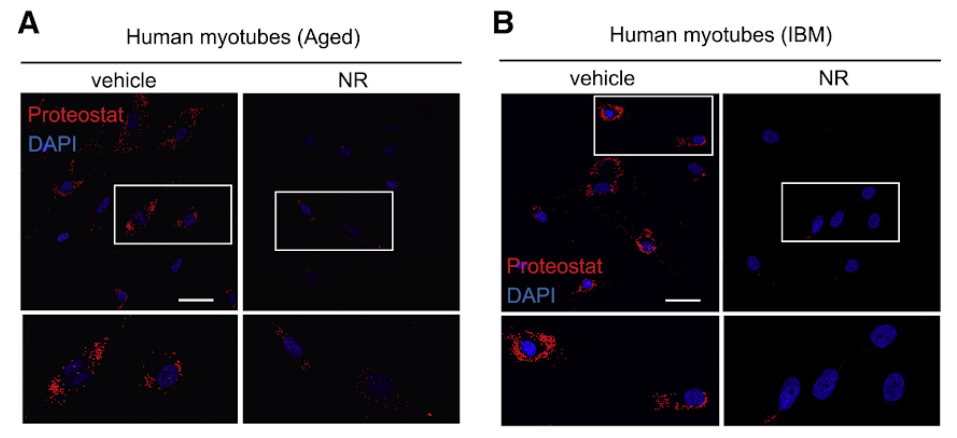
To translate the findings in worms to mammals, they also treated primary human myotubes obtained from aged subjects and IBM patients with NR and AZD and assessed the presence of amyloid-like proteins. Importantly, both treatments decreased the number of protein aggregates in cells derived from aged or IBM donors and mouse myotubes. Interestingly, co-treating cells with a drug called a global integrative stress response (ISR) inhibitor (ISRIB), attenuated the reduction in aggregates seen upon NAD+ boosting. The reduction of amyloid-like deposits was mirrored by an improvement of the mitochondrial membrane potential, increased mitochondrial respiration, and more fine network-like mitochondrial formations.
The future of restoring age-related muscle deterioration with NAD+
“Our results in [worms], mice, and humans support the notion that natural aging is typified by muscle amyloidosis and, very importantly, that late-life treatments aimed at restoring metabolic and mitochondrial homeostasis also increase cellular and organismal proteostasis, therefore beneficially impacting on health- and lifespan,” the authors concluded. Plus, NAD+ boosting improves proteostasis and attenuates amyloid formation across species, including humans.
The promising outcomes of this study could trigger clinical trials to test the efficacy of NAD+ therapeutics in human diseases related to amyloidosis. Future work may focus on finding the ideal NAD+ boosting strategy by testing different precursors besides NR, such as Nicotinamide Mononucleotide (NMN).
*Special note - This article is for informational purposes only and cannot replace a doctor's treatment diagnosis and advice. It should not be regarded as a recommendation or proof of efficacy of the medical products involved. If it involves disease diagnosis, treatment, and rehabilitation, please be sure to go to a professional medical institution to seek professional advice.
Previous: NMN Reduces Metabolic Impairment in Male Mouse Offspring from Obese Mothers
Next: Study Shows that NAD+ Precursors Reversion Blood Vessel Dysfunction
by GSHWORLD
GSH Bio Tech is China Biological API Manufacturer. China NAD+ powder suppliers & best NAD+ raw material Factory.














